

ECOSHELTA has long been part of the sustainable building revolution and makes high quality architect designed, environmentally minimal impact, prefabricated, modular buildings, using latest technologies. Our state of the art building system has been used for cabins, houses, studios, eco-tourism accommodation and villages. We make beautiful spaces, the applications are endless, the potential exciting.
By T. Murat. Defiance College. 2018.
In summary discount bupron sr 150 mg free shipping depression symptoms female, this technique of ultrasound measurement is best used to femur cheap 150mg bupron sr otc depression is a disease. The amount of internal rotation is now measured by using the tibia as the angle monitor children who have not had previous surgery if physicians feel this guide. Fluoroscopy Another technique for measuring femoral anteversion is with fluoroscopy. This technique involves observing the proximal femur and identifying that point when the amount of rotation of the femur has the anteroposterior pro- jection of the proximal femur in its best profile. In this position, the degree of internal rotation is measured with the knee flexed, demonstrating the degree of femoral anteversion. Other techniques using fluoroscopy have made radiographic images with the knee in its direct anteroposterior plane and then made a radiographic image with the hips in- ternally rotated until the proximal femur is in full sagittal plane profile. Us- ing triangulation, the difference in the length of the femoral neck is assessed to calculate anteversion. This technique does exactly the same thing as meas- uring the degree of internal rotation directly, but it adds the complexity and measurement errors inherent in having to measure the radiographs. Fluoroscopy is the ideal mechanism for measuring an- teversion in the operating room when hip reconstruction is contemplated. In this situation, the fluoroscope is available in the standard operating proce- dure and checking the degree of anteversion and getting an accurate assess- ment of proximal femoral coxa valga adds no additional time. Magnetic Resonance Imaging Scan One study reports using magnetic resonance imaging (MRI) scan to meas- ure femoral anteversion and documents that the MRI scan has the same accuracy and problems inherent with CT scan. No other major benefits are known, and certainly the bone image is never quite so good on MRI scan as it is on CT scan. Measurement Summary There are many methods for measuring femoral anteversion and femoral neck shaft angle, each measuring slightly different things and having some variation in the degree of accuracy. There is no consensus about which tech- nique for measuring femoral anteversion is the best, and as noted previously, each has its drawbacks and benefits. There also is no consensus about when femoral anteversion and coxa valga need to be measured accurately. For most of the children being followed, the assessment of femoral anteversion can be done accurately enough by continuing to monitor the physical ex- amination of the internal and external rotation of the hip and occasionally adding the palpation of the lateral trochanter measurement. For research projects in which more accurate measurements of the influence of femoral anteversion on a deformity are necessary, we believe more accurate imaging methods are required. The use of ultrasound is easy, sufficiently accurate, and inexpensive to use for those children who do not have severe deformi- ties and who have not had hip surgery. In more complicated patients who have had hip surgery and have developed recurrent internal rotation, it is often not clear exactly where this deformity is coming from (Case 10. There is often a concern of recurrent or residual uncorrected anteversion be- ing present. In these individuals, the best method for measuring anteversion is the CT scan because low to normal neck shaft angle is usually present as these children already had the coxa valga corrected. The irregular surfaces of the femur can be more easily dealt with by having a whole outline of the proximal femur, which is provided by the CT scan. In the operating room, using the fluoroscope to understand coxa valga and femoral anteversion is routine as part of the operative procedure. However, it is not necessary to make an absolute measurement of the degree of femoral anteversion pre- operatively in all children who have severe internal rotation and are being brought to the operating room to have this corrected. If children have not previously had hip surgery, and are being scheduled for surgical correction of the internal rotation deformity of the femur, increased femoral antever- sion is the problem and measurement of the anteversion beyond the physi- cal examination is not routinely needed. The Etiology of Femoral Anteversion and Coxa Valga Femoral anteversion is a normal position of the femur in infants. Femoral anteversion varies from 40° to 60° at birth, and then slowly resolves with growth until the normal 10° to 20° of anteversion is reached by age 8 years. There is a significant variation in the magnitude of anteversion at birth. In children with spasticity, the normal resolution of this anteversion does not occur because the spasticity and poor motor control do not provide a me- chanical environment in which the femur derotates itself. In addition, chil- dren with spasticity who maintain this high degree of infantile anteversion often have decreased motor control, which means they have less ability to compensate for this tendency to internally rotate from the increased femoral anteversion. A second aspect that may magnify the persistent infantile femoral anteversion begins to show up in middle childhood with the develop- ment of internal rotation contractures, which further magnify the persistent 10. His parents were concerned about the severe internal rotation position of the left hip.
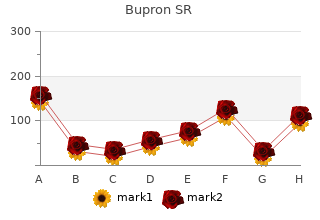
Usu- circumferential wrap can be used for many ally discount 150 mg bupron sr hdrs depression test, an anterior ankle strap is used quality bupron sr 150mg depression nos dsm 5; however, in some older children with good of the different designs. Its major limitation is that the thin plastic is weaker and gains ankle plantar flexion control, this is not needed. Also, the heel is typically strength by the circumferential wrapping na- posted on the side opposite the deformity. This means a lateral squaring of ture of the design. It does not work for high- the heel is added for varus deformity so the ground reaction force will tend stress environments, such as ground reaction to counteract the deformity. The opposite is done for valgus deformity, in AFOs, and can be difficult to put on and take which a post is added to the medial side of the heel. This supramalleolar foot off, especially for children just learning to orthotic design also works well with the wrap-around thin plastic design; how- dress themselves. It is more difficult for children to don the orthotic, and heavy children tend to collapse Figure 6. AFOs made for children the orthotic the same way a shoe deforms with long-term wear. There is no with spasticity need a good stable anterior ankle strap that is directed across the axis clear choice between the thin plastic wrap-around design and the solid plastic of the ankle joint. Input from the families and children should be considered is a padded anterior ankle strap that loops as well as the preference of the orthotists. Most children who need control through a D-ring fixed on the side opposite of planovalgus or varus, but have good plantar flexion and dorsiflexion con- the main deforming force (A). If the child has trol of the ankle, should be fitted with a supramalleolar orthotic (SMO). This orthotic contains a good to tighten the strap and allows the Velcro to heel mold, a medial longitudinal arch mold, a heel post, and typically stops hold better (B). These orthotics can be set into shoes, have no anterior ankle straps, and are very easy to don because they do not need to be removed from the shoe. Applying this orthotic is no more diffi- cult than putting on children’s shoes. The use of this orthosis in spastic foot deformities is limited because of its limited ability to provide corrective force. Another name that is used for this inframalleolar orthotic in some locations is a “University of California Biomechanics Laboratory” (UCBL) orthotic. The degree of contouring and molding of the plantar surface of the orthotic inspires a lot of discussion and strong feel- ings; however, objective data currently do not suggest that it makes much difference. The tone-reducing features are varied; how- ever, they tend to include some combination of transverse metatarsal arch, medial arch, peroneal arch, and transverse calcaneal arch (A,B). When comparing the relatively flat sole often used (C) with the highly contoured sole, there is minimal functional difference. The same benefit can also be obtained by adding pads to the inside of the orthotic using a soft B plastic (D). These pressure areas can also be molded directly into the orthotic. Some also like to square off the heel on the outside to give better control of the orthotic in the shoe (E). This feature makes application of the shoes harder than leaving the heel rounded, and less contouring on the toe plate allows easier extension of the orthotic as the child grows. Another technique used is to flatten the sole externally with a rubber material; how- C ever, this increases the height of the orthotic and makes shoe fitting more difficult (F). In-shoe foot orthotics are used primarily to control planovalgus or varus foot deformities. These can be constructed with The use of shoe inlay arch supports have little role in the management of the wrap-around design (A) or with the solid foot deformities in children with CP. The force of the collapsing foot is so plastic, which sits in the shoe (B).
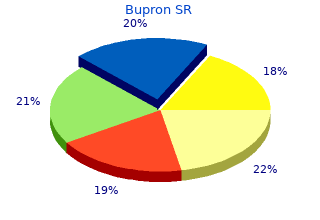
Parents are instructed to try to keep the child’s hips adducted bupron sr 150 mg cheap mood disorder and suicide, or if the release was for internal rotation buy cheap bupron sr 150 mg on line anxiety attack treatment, to keep the hips externally rotated during sleep at night. This should be accomplished with positioning, not with rigid braces. Resection Arthroplasty Indication This procedure is indicated as a palliative treatment to decrease the hip pain in nonambulatory children and adults with painful dislocated hips in which there is severe degenerative arthritis and deformity of the femoral head and ac- etabulum. It is the primary procedure in cases where there is skin breakdown. The incision is made over the lateral border of the femur carried down the subcutaneous tissue. The incision should extend distally from the tip of the palpable greater trochanter to approximately 6 or 8 cm (Figure S3. The fascia latae is incised longitudinally and then the vastus lateralis is identified. The fascia of the vastus lateralis is opened longitudinally; however, subperiosteal dissection of the femur should not be obtained. Using fluoroscopic control, the interval between the muscle and perio- steum is identified at the inferior aspect of the ischium. Using an oscillating saw, the femur is transected at this level (Figure S3. After the femur has been transected, the proximal femur is resected using electrocautery to avoid any subperiosteal dissection because leaving the periosteum tends to cause heterotopic ossification. All of the periosteum and proximal femur are resected with a slight sleeve of soft tissue with extensive use of electrocautery to help minimize bleeding. The hip joint capsule usually is resected right at the border of the femoral neck, leaving a sleeve of hip joint capsule associated with the residual acetabulum. The abductor muscle also is resected well off the tip of the greater trochanter so that no apophysis that might form bone is remaining. After the proximal fragment is removed, sutures are placed in an at- tempt to cover the rough and open bone on the ilium by suturing hip joint capsule and muscle over this area (Figure S3. The sleeve of vastus lateralis, which had been freed off the proximal fragment, is sutured over the top of the exposed bone on the distal fragment (Figure S3. The vastus lateralis then is closed tightly, subcutaneous tissue and skin are closed, and the child is placed in skeletal traction or a well leg cast with broomsticks between the legs to provide some traction and positioning. Well leg traction is a technique in which bilateral short-leg casts are applied and then are rigidly cross-connected with two strong broomsticks. This makes a rectangle so the leg that had the femoral resection is prevented from migrating proximal by the healthy leg. Postoperative Care The minimal postoperative care requires the use of the broomstick well leg casts or skeletal traction with distal femoral traction for 6 to 8 weeks. Some surgeons have recommended using external fixation but this seems to be an extreme method of applying traction in these severely compromised indi- viduals. Pain relief typically requires a minimum of 6 months, with many children requiring as long as 12 to 18 months to reach maximum pain relief. No effort is made to increase range of motion by therapy. Children should not be doing any weight bearing until there is maximum pain relief and then only minimal weight bearing is recommended. Interposition Arthroplasty Indication The interposition arthroplasty is another salvage procedure that can be used for the painful severely degenerated hip in nonambulatory children and adults. The goal is to implant a humeral component, which acts as a spacer so the individual gets immediate pain relief and does not have to wait 12 to 18 months as is typical for the resection arthroplasty. The incision is made on the lateral aspect of the femur from the tip of the greater trochanter to 10 cm distal (Figure S3. Subcutaneous tissue is opened in line with the skin incision. Fascia latae is longitudinally incised in the same line.

The battery that powers the pump has an implanted life ranging from 3 to 5 years buy bupron sr 150mg otc anxiety physical symptoms. When the battery loses power order bupron sr 150 mg overnight delivery depression after test e, the whole pump has to be replaced. If there is any question as to whether a child’s pump is functioning or there is a catheter malfunction, the child should be placed on oral baclofen to prevent the withdrawal psychosis that occurs in some children. Baclofen also has an antihypertensive effect31; however, this is seldom a significant problem. There may be a sympathetic blockade-type effect decreasing the overreacting peripheral basal motor response that creates blue feet when the feet get cold. In this report, a significant number of men reported a de- creased time and rigidity of erections, and two men reported losing the ability to ejaculate. This complication should be men- tioned to patients for whom it might be a concern. A small group of children require a very high dose of intrathecal baclofen, sometimes 2000 to 3000 mg per day. Also, some children who are on a lower dose suddenly need increased doses if their spasticity is increasing 6 months to 2 years after the implantation. If a child has had an increasing need for baclofen, or is requiring a sudden increase in baclofen after having been stable, catheter malfunction should be considered. After the full workup for catheter malfunction, or after demonstration that the catheter is function- ing, another option for dosing is to use a drug holiday. In this treatment, the intrathecal baclofen is reduced and then slowly decreased to zero to avoid a withdrawal psychosis. The pump may be left in the turned-off position for 1 month and then the drug slowly reintroduced. This drug holiday should allow the nervous system to redevelop a sensitivity to the drug. Another way to use this concept of a drug holiday is to give large intrathecal boluses sev- eral times a day instead of continuous dosing. Therefore, instead of giving a continuous dosing rate of 2000 mg, the child may be given 1000 mg just before bedtime, and then another 1000 mg over a 30-minute period the first thing in the morning. These different dosing regimens may provide a better benefit in some children compared with continuous administration. The current role of intrathecal baclofen in the treatment of children with severe spasticity is primarily in nonambulatory children. From a theoretical standpoint, this treatment should also be ideal for the 3- to 8-year-old spas- tic ambulatory child for whom a rhizotomy could be considered. The size of the pump and the need for long-term maintenance, with filling at least every 3 months, has made it difficult to convince parents and physicians that this is a good treatment option. Also, there are no objective published data that allow one to develop confidence. This question would be an excellent project for a well-controlled study similar to the randomized rhizotomy studies. As better engineered pumps are designed and medication that has more stability is found, so that the pump only needs to be filled every 6 months to 1 year, the intrathecal pump will become an even better option, especially for high-functioning children. Also, there are other medications that may be even better choices than baclofen; however, each of these needs to be trialed and tested in children with spasticity. Neurologic Control of the Musculoskeletal System 115 Rhizotomy Central nervous system surgical approaches to reducing spasticity are most commonly done at the spinal cord level, with posterior dorsal rhizotomy be- ing the most widely used procedure. This procedure involves cutting the dorsal sensory nerve rootlets, which contain the afferent sensory nerves, from the muscle spindles as well as other sensory nerves. By using peripheral motor stimulation and recording the electrical activity in the proximal sen- sory nerves, abnormal rootlets are identified and then sectioned. Many rootlets are not quite normal or not very abnormal, which makes choosing the abnormal ones very subjective. Evidence exists that there is no difference between selective nerve sectioning based on electrical stimulation and just random sectioning. The operative procedure may be done as popularized by Peacock et al. There is no apparent differ- ence between outcomes of the two procedures based on published reports; however, the Peacock technique is more popular in North America.