

ECOSHELTA has long been part of the sustainable building revolution and makes high quality architect designed, environmentally minimal impact, prefabricated, modular buildings, using latest technologies. Our state of the art building system has been used for cabins, houses, studios, eco-tourism accommodation and villages. We make beautiful spaces, the applications are endless, the potential exciting.
By H. Marius. William Woods University. 2018.
A second concern is that patients with a history of addiction may relapse suprax 200mg amex bacteria urine test results. A person with risk factors for developing a SUD buy generic suprax 100 mg on-line infection kansen, such as certain psychiatric diagnoses or a family history of addiction, may misuse, abuse, or become dependent upon the prescribed drug [40, 41]. Several assessment tools have been presented in the chronic pain literature that may assist in identifying patients who are at risk of addiction. Toxicology screening and a thorough clinical To Help and Not to Harm 157 Table 3. Risks of treating chronic pain in SUD Biological risks Dependence Tolerance Withdrawal Clinical risks: patient oriented New SUD Relapse of prior SUD Legal risks: physician oriented Professional censure Legal sanction Psychosocial risks: physician–patient relationship Manipulation of relationship Exploitation of the system Diversion of controlled substances Countertransference reactions interview may also improve the clinician’s ability to prospectively identify patients who may have or develop an addiction. If these methods are used to bar patients from opioid and other effective therapies, then they may them- selves cause harm to the patient. If on the other hand, they are used as their authors intend, to anticipate the needs of patients with predisposition to addic- tion and to enable clinicians and patients to marshal other resources to support the patient during treatment, then they reduce the harms both of not treating chronic pain and of iatrogenic relapse or addiction. A third issue confronting clinicians are medical-legal barriers to opioid treatment which arise in the setting of addictive drug use. Physicians fear that if they prescribe controlled substances to patients with known histories of addiction or current SUD, they may be liable to professional censure or legal sanction. Research shows this results in inadequate treatment of chronic pain in patients with SUD. They found that 226 of these patients reported per- sistent or frequent pain during the 2 weeks prior to the survey. Nearly 85% of patients with pain were receiving inadequate medication according to the Pain Management Index. Those most likely to be receiving inadequate treatment were women, less educated patients, and patients who had contracted HIV through IVDU. While physicians have some justification for their anxiety about the use of chronic opioids, there also have been legal repercussions for under- treatment of pain. A California jury found a physician guilty of elder abuse for undertreating pain. The duty of a physician to treat despite legal issues has received recognition in the various physician organizations. According to the Geppert 158 Principles of the American Medical Association, ‘A physician shall respect the law and also recognize a responsibility to seek changes in those requirements that are contrary to the best interests of the patient’. Implicit in this charge is that a physician’s clinical judgment be informed by an accurate, up-to-date knowledge of federal and state legislation relevant to the prescription of con- trolled substances in patients with addiction. This enjoins physicians to be invested in political action that will influence policy that undermines good medical practice. The rein- forcing effects of opioids may have the effect of exacerbating disability and worsening relationships for patients. The ethical intent of opioid prescribing must be to improve prosocial functioning, including behavior related to the clinical encounter. This becomes most clear when the patient develops behav- iors that disrupt the doctor–patient relationship. The critical incident study referred to earlier found that physicians experienced the ethical dilemmas sur- rounding opioid prescription as stressful encounters that had a negative impact on self-esteem and represented a failure in the physician-patient relationship. Patients who display problematic behavior, such as lying to physicians about illicit drug use or doctor shopping, trigger countertransference reactions of frustration, resentment, and fear of being manipulated. These reactions are well documented in the difficult patient literature and are a long-established field of expertise for consultation-liaison psychiatry. Pain specialists and primary care physicians who provide the majority of chronic pain treatment often do not have the training to manage these behaviors. Physicians who experience ethical dilemmas regarding prescription of controlled substances have identified education in the pharmacology of pain management, addiction treatment, and communication skills as crucial to constructively managing countertransference reactions and maintaining the integrity of the physician– patient relationship. The much quoted discussion of pseudoaddiction of Weissman and Haddox underscores this point. Patients with or without a history of addiction, who receive inadequate pain medication, may respond with ‘pseudoaddictive behav- iors’ such as unauthorized dosage increases and/or visiting multiple physicians leading physicians to suspect abuse and perhaps reduce medication, creating a vicious cycle. Responding to addictive behaviors in pain patients as if they were addicts can deprive the patient of the benefits of effective pain medica- tion and cause additional harms of stigmatization, and the delivery of a poor quality of medical care obtained through the emergency room or from multiple providers.
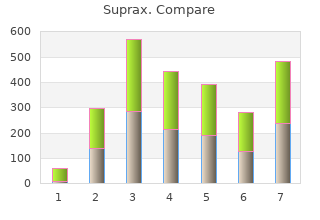
The pivot point of even very complex correc- tions can be precisely adjusted purchase 100mg suprax mastercard antibiotic treatment for h pylori. In order to shorten the application period of the fixator cheap 200 mg suprax amex zyvox antibiotic resistance, and thus the associated handicap, we replace the frame after the desired length has been achieved and callus has started to form with a specially produced Tomofix plate. This plate has fixed-angle screws, does not lie completely flush against the periosteum (and does not therefore impair the circulation) and has a relatively high intrinsic elasticity (thereby promoting callus formation). Complications Surgical leg lengthening and deformity correction are pro- tracted, unpleasant treatments that are demanding for all involved and full of complications. Parents and child must be fully briefed accordingly before the start of treatment. Reputable studies have shown that every patient suffers one fairly major complication on average [7, 12, 20, 21, 32, 38]. For the femoral orthopaedists like to differentiate between »complications«, lengthening we use a monolateral fixator with a hinge (arrow), which »problems« and »obstacles«. We do not consider these allows continuous axial correction euphemistic terms to be particularly useful and therefore ⊡ Fig. Photograph of the Taylor Spatial Frame on the lower leg of a 15- year old boy with achondroplasia and varus deformity of the lower leg and excessively long fibula with shortening of the tibia 567 4 4. Major complica- tions are those that require an unscheduled operation, whereas minor complications can be solved without an operation. The principal complications are as follows: ▬ Superficial infections at the entry points of the Kirsch- ner wires or screws. Such infections occur in almost all patients and can be treated by corresponding care, bathing and occasionally by antibiotic administration or a small incision. The entry points must not only be disinfected every day, it is also important that the chil- dren take regular baths. Soaking in water helps avoid crust formation and the retention of bacteria with consequent infection. Far from constituting an infec- tion hazard, the bath water actually helps avoid infec- tions. The nail entry points must also be adequately cleaned mechanically, since the disinfectant on its own is ineffective. If it occurs during lower leg lengthening there is a risk of an increasing equinus foot position. This tendency can be counteracted with physiotherapy, splints and ban- dages (⊡ Fig. If neighboring joints are particu- larly at risk they must be included in the assembly ⊡ Fig. Angulation corrections also involve cur especially if those joints are at risk, i. This is Nerve lesions – at least those with significant impact usually only possible with ring fixator systems. Nevertheless, they can ening of longer segments and can be predicted on even occur at this lengthening rate. The angulation is always Fractures occur particularly after the removal of the in the varus direction at the proximal femur and in external fixator. They can occur in the lengthened the valgus direction at the distal femur and the tibia. Angulations can be avoided by the use of a ring fixator But fractures can also occur elsewhere on the length- (e. For this reason weight-bearing is ▬ Pain of varying degrees can be expected in all length- extremely important. Alman BA, Krajbich JI, Hubbard S (1995) Proximal femoral focal bit tibia after callotasis. J Bone Joint Surg (Br) 75: 898–903 deficiency: Results of rotationplasty and Syme amputation. Luke DL, Schoenecker PL, Blair VP, Capelli AM (1992) Fractures Bone Joint Surg (Am) 77: 1876–82 after Wagner limb lengthening.
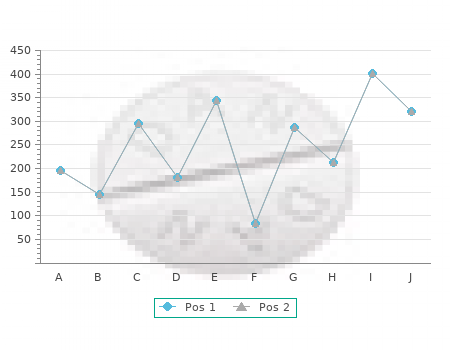
At this point buy discount suprax 200mg virus replication cycle, I usually affix one side of the graft with staples and maximally expand the graft in the other directions best 200mg suprax antibiotics for ear infection. Grafts can then be applied adjacent to this as required for wound closure. When using 4:1 or 9:1 mesh ratios, the wound will still be mostly open after application of the autograft. At this point, we advise that the wound be completely closed by application of cadaveric homograft over the autograft (Fig. When using this technique, staples are not applied until all layers of the skin are in place. With successful graft take using this technique, the autograft and homograft become adherent and vascularized. With time, the homograft cells reject while the autograft cells expand, thus completing wound healing. Selection of the donor sites, mesh ratio, and placement of the grafts com- prise the majority of the art of burn surgery. The wound bed can be viewed as a puzzle, and the autograft as pieces of it. The advantage of this model is that the pieces can be cut to fit the puzzle. However, efforts should be made to keep the pieces whole in order to minimize seams. Application of Dressings Once the grafts are in place posteriorly, dressings should be applied. In areas that are dependent such as the back and the buttocks, tie-over bolsters should be placed to minimize shearing. Sutures should be placed in such a way that a geometric shape results when they are tied (rectangles or squares work best). In the case of a wound bed that goes around to the anterior trunk, it is only necessary to bolster to the posterior axillary line. Once the sutures are in place, a layer of one-half polysporin 1% ointment and one-half nystatin 1% ointment (polymyco)-impregnated fine-mesh gauze should be placed over the wound. Several layers of cotton gauze (5–6cm) are placed over this, and the sutures are tied over all this firmly so that the dressing does not slide. In the case of the buttocks, polymyco gauze should be wrapped over the cotton gauze to minimize soiling. The legs do not require bolsters, because they can be wrapped circumferentially once the patient is in the supine position. I generally do not apply any dressings at all on the legs until the patient is placed back in the supine position. This is accomplished by disconnecting the monitors again and covering the patient with a clean drape. The patient is then rolled back into the arms of two members of the surgical team at the shoulders and hips. The patient is lifted completely off the bed, the hip and ankle rolls are removed, and the patient placed back onto the shoulder roll as the monitors are reconnected. Attention is then given to placement of the grafts anteriorly on the legs, perineum, and trunk. Simultaneous with this, the arms are elevated with hooks 242 Wolf (as described above), and the excision carried out on them. Dressings are applied as previously mentioned on the trunk, but bolsters are not necessary. The limbs are dressed with circumferential strips of polymyco gauze followed by layers of cotton gauze and an elastic bandage. This can be done by the surgeon with plaster or fiber glass placed posteriorly followed by another elastic bandage. As an alternative, splints can be applied with Ther- moplast in the recovery room by either the surgeon or experienced occupational and physical therapists. The Surgical Team For these operations to be done in a timely manner requires at least two experi- enced surgeons, and up to four are preferable. The senior surgeon makes decisions regarding the adequacy of excision, which donor site areas will be taken, and how the skin will be meshed and where it will be placed.
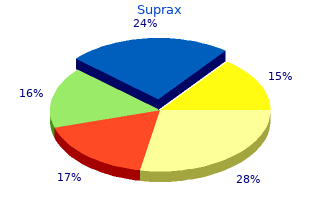
When patients are scheduled for surgery generic 100mg suprax overnight delivery antibiotics just in case, nutrition is stopped 2–4 h before surgery buy suprax 200 mg on line virus y antivirus, and the stomach is aspirated prior to the induction of anesthesia. In ventilated patients, enteral nutrition is not stopped but is contin- ued during surgery. Caloric requirements in burn patients should be ideally calculated by means of indirect calorimetric measurement. After measurement of the composition of expired gases, the calorimeter calculates the respiratory quotient and caloric requirement by means of standard equations. When indirect calorimetry is not available, calorie requirements are measured calculated on linear regression analysis of intake vs. Patients should be assessed for nutritional status on admission, and reassessed on a daily basis. It is also important to determine whether the regimen is well tolerated. Patients should be investigated with a complete nutritional panel on admission and then once a week. This includes: Total lymphocyte count, white blood cells, hemoglobin and hematocrit, and mean corpuscular volume TABLE 1 Initial Nutritional Assessment Determine the caloric and protein needs of patients immediately upon admission Assessment by physician and dietician Assess: – Personal background – Chronic conditions – Hypermetabolic conditions – Physical conditions that may interfere with food intake – Predisposing factors – Recent weight loss or gain – Food preference and allergies – Weight and height for age and gender – Total lymphocyte count – White blood cells – Hemoglobin and hematocrit – Mean corpuscular volume Perform indirect calorimetry if available Calculate daily calorie and protein needs 36 Barret Albumin, prealbumin, magnesium, phosphate, ionized calcium, copper, zinc, protoporphyrin/heme 24 h total urea nitrogen Measurement of these variables, together with indirect calorimetry and the weight gain/loss of the patient will give a good estimate of his or her nutritional status. Burn patients who can eat normally receive a high-protein, high-calorie diet. Liquids should be supplemented in the form of high-calorie fluids, such as milk or commercial milkshakes. Patients with burns over 25% BSA burned cannot cope with the caloric demands that trauma imposes on them, so that in all of them enteral supplementation is indicated. The most popular ones (Curreri and Harris Benedict for adults, and Galveston formula for children) are summarized in Table 2. Some of them (Curreri) may overestimate calorie requirements, whereas others (Harris-Benedict) may underestimate these needs. Therefore, they should be used as initial estimates, with patients needs titrated to their hypermetabolic response as measured by indirect calorimetry. It must be noted, however, that human hypermetabolic response reaches a maximum of about 200% of basal requirements. Above that, human physiology cannot increase the rate at which the fuels are utilized to transform them into energy and proteins. It means that supplementing above the 200% resting energy expenditure (REE) does not in- crease the absorption of nutrients. There is general agreement that this increase to 200% REE reaches the maximum with burn at or over 50% BSA. Approximately 50% TABLE 2 Nutritional Formulas Nutritional formulas for pediatric burn patients 0–12 months: 2100 kcal/m2 surface area 1000 kcal/m2 surface area burned 1–11 years: 1800 kcal/m2 surface area 1300 kcal/m2 surface area burned 12 years: 1500 kcal/m2 surface area 1500 kcal/m2 surface area burned Nutritional formulas for adult burn patients Curreri: 16–59 years: 25 kcal/kg 40 kcal for each percentage of burn area 60 years and more: 20 kcal/kg 65 kcal for each percentage of burn area Harris-Benedict: Basal energy expenditure (BEE) in kcal/day (at rest): Males: BEE 66 13. For a balanced daily diet, administration of vitamins C, A, and E, B complex, zinc, iron, folate, and trace minerals is essential. When the patient’s wounds are virtually covered, the diet should transition from one in which the majority of the nutrition is supplied via tube feedings to a total oral diet. Reduce tube feedings to a rate that with the oral intake equals 100% of reassessed goal. As oral intake increases, provide only nocturnal tube feedings to equal 100% of goal. When oral intake is at least 50% of goal, begin 3 day trial of oral diet with tube feedings held. If goal is not being met at the end of the trial, re-evaluate feeding methods and, if necessary, resume tube feedings. During all of the above steps, specific fluid orders with guidelines as to amounts and contents should be written PATIENT SUPPORT Hypoproteinemia and Anemia Hypoproteinemia due to malnutrition, continuing serum protein losses, and post- burn sepsis and hepatic dysfunction will persist until wound closure is achieved. Intravascular proteins can be replaced by processed albumin (generally preferred), or fresh frozen plasma if a significant coagulopathy is also present. The efficacy of colloids is the subject of debate; therefore every effort should be made to correct hypoproteinemia with early enteral nutrition. Colloids should be reserved for patients with severely low protein levels and those with significant clinical effects of such hypoproteinemia. The initial thermal injury is accompanied by direct destruction of red cells. Other cells are not initially destroyed, but they are structurally damaged and the half-life of the red cell pool is significantly decreased.
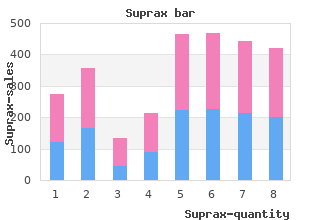
The chapter also provides coverage of various ethical concerns that are unique to the field of pain buy 100 mg suprax with visa antibiotic resistance of streptococcus pyogenes, as well as an overview of con- cerns that are especially relevant to psychologists generic suprax 200 mg mastercard antimicrobial face masks. We hope that the views presented herein will provide both a better ap- preciation of state-of-the-art developments in the psychology of pain and a greater appreciation of the richness and complexity of the pain experience. Sex-related differences in the effects of morphine and stress on visceral pain. Prevalence of chronic pain in the British population: A telephone survey of 1037 households. Gender differences in pain ratings and pupil reactions to painful pressure stimuli. An application of behavior modification tech- nique to a problem of chronic pain. A theoretical framework for understanding self- report and observational measures of pain: A communications model. Sensitivity to cold pressor pain in dysmenorrheic and non-dysmenorrheic women as a function of menstrual cycle phase. Montreal: Canadian Consortium on Pain Mechanisms, Diagnosis and Management. Abdominal pain and ir- ritable bowel syndrome in adolescents: A community-based study. International Association for the Study of Pain Ad Hoc Subcommittee for Psychology Curricu- lum. The tragedy of dementia: Clinically assessing pain in the confused, non- verbal elderly. Sensory motivational and central controlled determinants of pain: A new conceptual model. An epidemiologic analysis of pain in the elderly: The Iowa 65+ Rural Health Study. Sex differences in the an- tagonism of swim stress-induced analgesia: Effects of gonadectomy and estrogen replace- ment. Gender differences in pain per- ception and patterns of cerebral activation during noxious heat stimulation in humans. Expressing pain: The communication and interpretation of facial pain signals. Some embryological, neurological, psychiatric and psychoanalytic impli- cations of the body scheme. CHAPTER 1 The Gate Control Theory: Reaching for the Brain Ronald Melzack Department of Psychology, McGill University Joel Katz Department of Psychology, Toronto General Hospital Theories of pain, like all scientific theories, evolve as a result of the accumu- lation of new facts as well as leaps of the imagination (Kuhn, 1970). The gate control theory’s most revolutionary contribution to understanding pain was its emphasis on central neural mechanisms (Melzack & Wall, 1965). The the- ory forced the medical and biological sciences to accept the brain as an ac- tive system that filters, selects, and modulates inputs. The dorsal horns, too, were not merely passive transmission stations but sites at which dynamic ac- tivities—inhibition, excitation, and modulation—occurred. The great challenge ahead of us is to understand how the brain functions. A BRIEF HISTORY OF PAIN IN THE 20TH CENTURY The theory of pain we inherited in the 20th century was proposed by Des- cartes three centuries earlier (see Melzack & Wall, 1996). Descartes was the first philosopher to be influenced by the scientific method that flourished in the 17th century, and he achieved a major revolution by arguing that the body works like a machine that can be studied by using the experimental methods of physics pioneered by Galileo and others. Although humans, Descartes proposed, have a soul (or mind), the human body is nevertheless a machine like an animal’s body. The history of experi- ments on the anatomy and physiology of pain during the first half of the 20th century (reviewed in Melzack & Wall, 1996) is marked by a search for specific pain fibers and pathways and a pain center in the brain. The result was a concept of pain as a specific, straight-through sensory projection sys- tem (Fig. This rigid anatomy of pain in the 1950s led to attempts to treat severe chronic pain by a variety of neurosurgical lesions. Descartes’s specificity theory, then, determined the “facts” as they were known up to the middle of the 20th century, and even determined therapy. Specificity theory proposed that injury activates specific pain receptors and fibers, which, in turn, project pain impulses through a spinal pain path- way to a pain center in the brain.